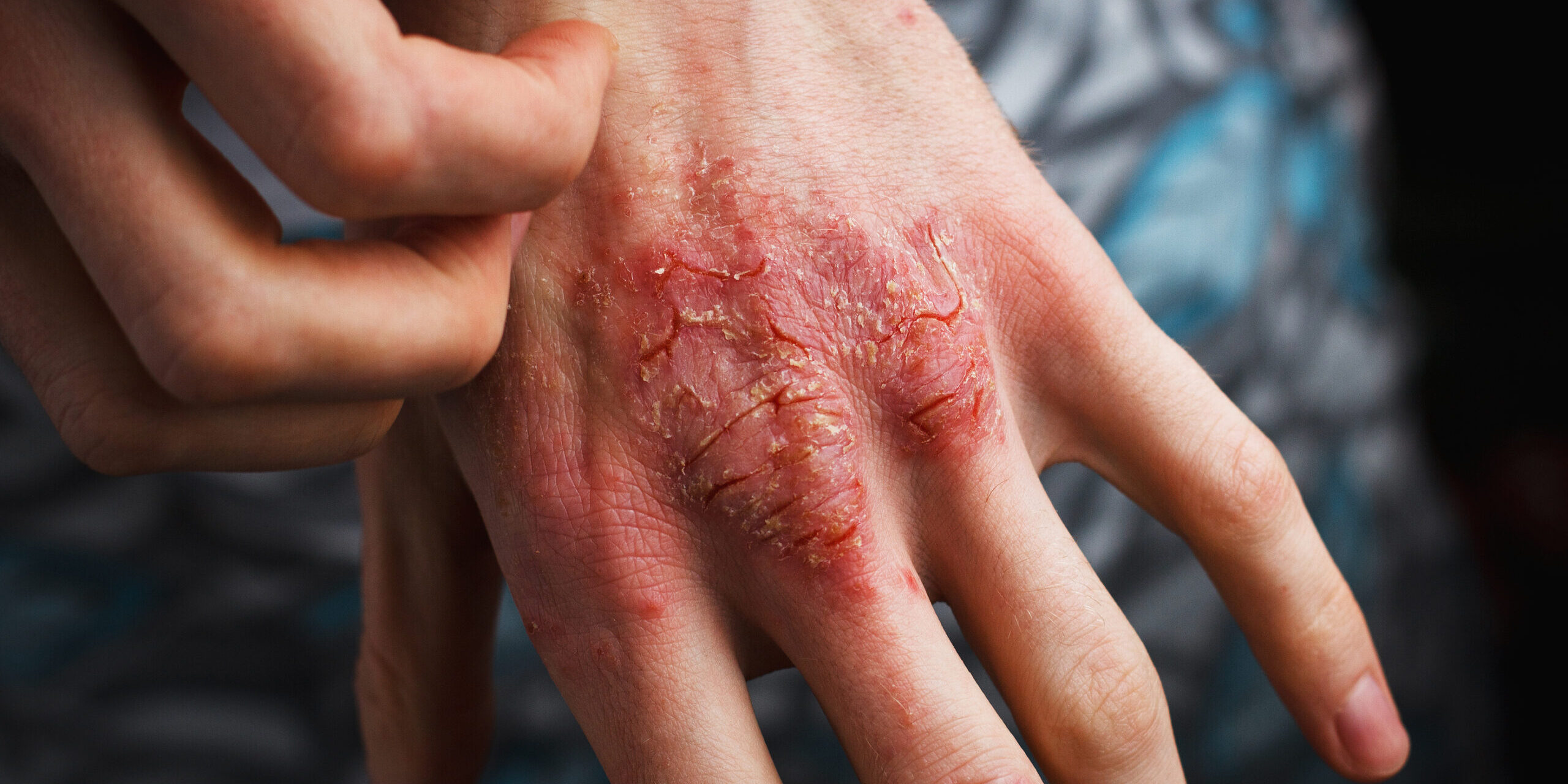
Psoriasis is a chronic autoimmune condition that impacts more than 7.5 million Americans. A decade ago, getting a patient 50% clear of a flare was considered a success. But now, Molly Sarkis, MMS, PA-C, of Apex Skin’s Medina location, aims for 90, thanks to how dramatically treatment has advanced.
It’s not uncommon for patients to live with psoriasis longer than they need to, making quiet sacrifices like sitting out summers, avoiding the salon, covering up. Sarkis wants patients to know that there is help and that what’s possible today looks a lot different than it did ten years ago.
What Exactly Is Psoriasis?
Psoriasis is a chronic autoimmune condition, which means the immune system is overworking, producing too many skin cells and triggering a rash. Because the immune system is the driver, psoriasis doesn’t stay at the surface, sometimes causing inflammation in the joints, gut, and cardiovascular system. While there’s no cure, the right treatment plan can effectively manage psoriasis.
Psoriasis can appear at any age, but it most commonly follows a bimodal pattern: a first peak between ages 20 and 40, and a second between 40 and 60.
Psoriasis Symptoms: What You Might Notice
Most patients see a dermatologist because of a rash, but symptoms depend on the type of psoriasis involved.
- Plaque psoriasis is the most common form. It can appear anywhere on the body but shows up most often on the scalp, elbows, knees, and the gluteal cleft. Its defining characteristic is a sharp, well-defined border with skin that is typically red, raised, inflamed, and scaly.
- Guttate psoriasis appears as small, scattered spots rather than defined plaques and is seen more often in children, though any age group can be affected. About half the time, it follows an infection like strep throat or an upper respiratory virus. In some cases it resolves on its own; in others, it progresses to plaque psoriasis over time.
- Inverse psoriasis affects the skin folds: behind the ears, the armpits, under the breasts, the abdominal fold, and the groin. Unlike plaque psoriasis, it tends to be smooth and shiny rather than raised and scaly, often causing small cracks in the skin that can be painful.
- Nail psoriasis is something patients frequently mistake for a fungal infection. Signs include pitting, discoloration, thickening, and the nail lifting away from the nail bed. When the diagnosis is unclear, a nail clipping can confirm whether fungus is present.
- Pustular psoriasis most commonly affects the palms and soles of the feet, producing small whiteheads on the skin alongside peeling. A generalized form, where the whiteheads spread across large areas of the body, exists but is rare.
- Erythrodermic psoriasis is the most severe form with widespread redness covering much of the body, often accompanied by pain and fever. It’s uncommon and is a medical emergency requiring hospitalization and aggressive systemic treatment. Patients who experience sudden, widespread skin redness should seek immediate care.
- Psoriatic arthritis is a related condition affecting the joints, occurring in up to 30% of people with psoriasis. In rare cases, it can develop without any skin involvement at all.
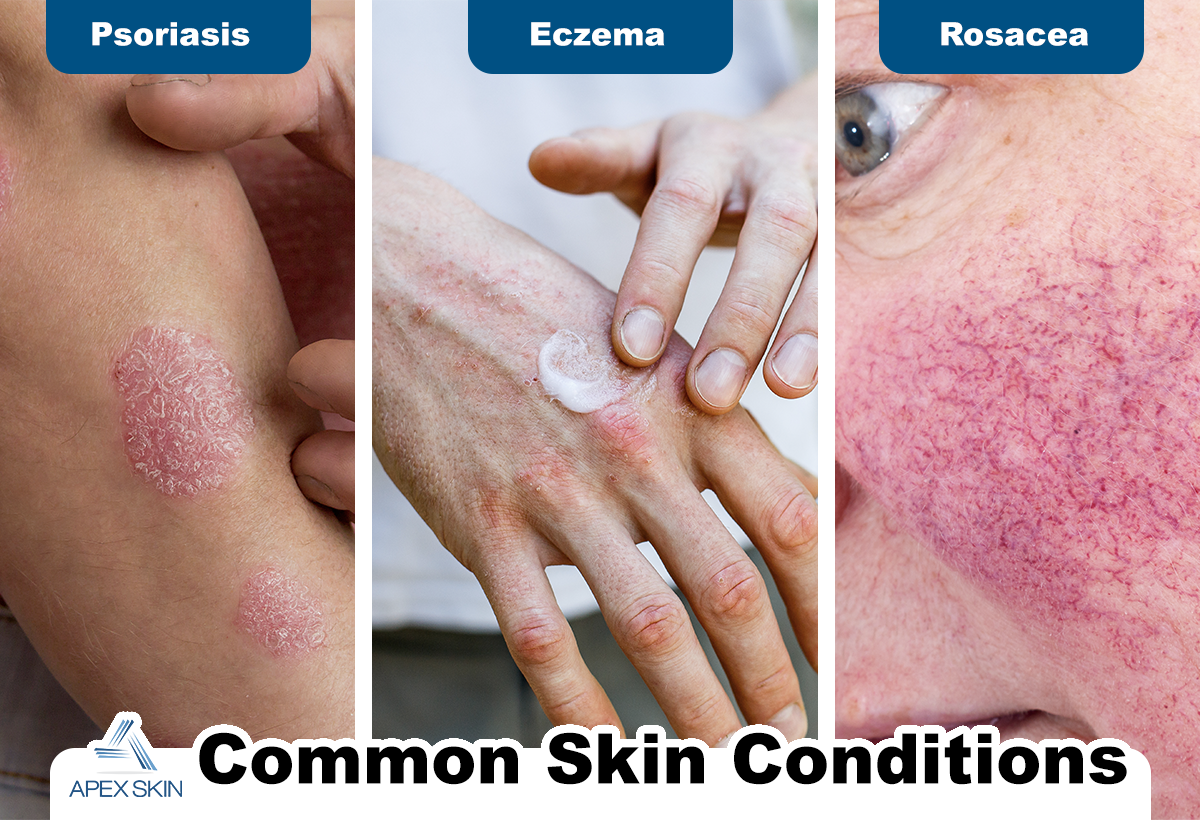
Psoriasis vs. Eczema: How to Tell the Difference
The clearest distinguishing feature of psoriasis is a sharp, well-defined border. Eczema typically lacks it, and while both conditions can be scaly, eczema tends to be less raised. That said, the two can be genuinely difficult to tell apart and the distinction matters when it comes to treatment.
When the diagnosis is unclear, Apex Skin has a significant advantage: an in-house dermatopathology lab at the Mayfield Heights location. A skin biopsy can be taken, examined under a microscope, and used to confirm whether what’s present is psoriasis, eczema, or something else entirely so that the right treatment path is clear from the start.
What Triggers a Psoriasis Flare?
Understanding your triggers is one of the most useful things you can do for long-term management.
- Stress is the most common trigger, and Sarkis means that broadly—emotional stress from work or loss, but also physical stress on the body like surgery or illness.
- Wintertime is another consistent pattern, driven by cold dry air, reduced sunlight, and drier skin overall.
- One trigger that surprises many patients: certain medications. Beta blockers, commonly prescribed for heart rate or blood pressure, are a well-known psoriasis trigger.
- Other triggers include infections, smoking, alcohol, and skin trauma. Even a sunburn or a scratch can set off a flare.
What most psoriasis triggers have in common is that they place additional stress on the body, internally or externally. Supporting your body through general inflammation—through sleep, diet, movement, and avoiding known irritants—is one of the most consistent things patients can do between flares.
“Telling someone to decrease stress is a lot easier said than done,” Sarkis admits. “But you can start with the basics. If you try to start big, it’s just too overwhelming and you give up.”
More Than a Skin Condition
Because psoriasis is driven by systemic inflammation, it doesn’t stay at the surface. Newly diagnosed patients are often surprised to learn how much is connected.
Psoriatic arthritis is one of the most important things to watch for. It affects up to 30% of people with psoriasis, and the joint damage it causes isn’t reversible once it sets in. Sarkis screens for it early, because catching it before damage accumulates changes what’s possible.
The signs are specific: swollen or tender fingers and toes, joint pain that doesn’t resolve within 30 minutes of waking up, and pain that tends to be one-sided.
“When you have psoriatic arthritis and the psoriasis starts to damage the joints, that’s not reversible,” she says. “We can stop the progression, but we can’t repair them once it’s occurred.”
Psoriasis is also associated with cardiovascular disease, metabolic syndrome, and depression—downstream effects of chronic systemic inflammation that go well beyond what a topical cream can address.

The Emotional Weight of Psoriasis
The clinical picture of psoriasis is well documented. The emotional side of it is talked about less. But in Sarkis’s exam room, it comes up constantly.
Patients cancel vacations. They avoid shorts all summer. They plan treatments around weddings. Behind those decisions is something more persistent: the fear that other people will think the rash is contagious, or that it reflects something about hygiene.
“I know, and my patients know, it’s not a hygiene issue and that it’s not contagious… it’s something that your body does all on its own,” Sarkis explains. “But other people don’t always know that.”
Itching that disrupts sleep, flaking that shows up on clothing, visible plaques on the hands and scalp are things that affect quality of life in ways that matter and Sarkis takes them seriously as part of the treatment conversation.
Psoriasis Treatment Options
The treatment landscape for psoriasis has changed significantly.
“We used to look at getting patients 50 or 75% clear,” Sarkis says. “Now we’re looking at getting them 90% clear.” A shift is worth knowing about especially for patients who may have tried treatment years ago and gave up.
- Topical treatments are typically the starting point for mild or localized psoriasis. These include topical steroids, vitamin D analogs that help reduce excess skin cell buildup, and newer non-steroid options like Vtama and Zoryve that can be used longer term without the limitations that come with steroid-based creams.
- Oral medications include newer options like Otezla, Sotyktu, and Iktvez —a recently approved addition to the category—alongside older systemic medications like methotrexate and cyclosporine, which Sarkis uses more selectively given the newer options now available.
- Biologics are injectable medications, typically administered at home using an auto-injector on a schedule ranging from every four to every twelve weeks. They target specific parts of the immune system driving the inflammation and are among the most effective options for moderate to severe psoriasis and psoriatic arthritis.
How Sarkis decides where to start depends on how much of the body is affected, which areas are involved, whether joint symptoms are present, and what the patient is comfortable with. It’s a decision she makes together with the patient.
Hands, feet, scalp, and nails tend to warrant more aggressive treatment even when the affected area is small, because of how significantly they affect daily function. For patients who come in extensively covered, topicals alone aren’t realistic or sufficient.
Living Well with Psoriasis
Treatment is the foundation, but lifestyle plays a real supporting role. Sarkis frames lifestyle changes as something to layer in as treatment starts working, not as a prerequisite to getting better.
Smoking cessation, reducing alcohol intake, eating an anti-inflammatory diet, and consistent movement all contribute to better disease control. The relationship between weight and psoriasis runs in both directions—obesity can trigger psoriasis, and psoriasis can contribute to weight gain. But what’s clear is that improvement in one tends to support improvement in the other.
The gut-skin connection also comes up in practice. One of Sarkis’s patients had localized psoriasis that kept reflaring despite topical treatment. After identifying and removing a few inflammatory foods from their diet, they were able to get the condition under control and eventually stop the topicals without the immediate reflare that had been the pattern.
“Just by taking that out and continuing with the topicals, they were able to get the psoriasis under control and then stop the topicals and basically not reflare.”
A Message for Newly Diagnosed Patients
If you’ve just received a psoriasis diagnosis or you’ve been living with an undiagnosed rash, the most important thing to know is that you have options.
Psoriasis affects 7.5 million Americans. It’s common, it’s manageable, and it’s nothing to be embarrassed about. Some patients have spent years assuming nothing could be done because treatment failed them once, long ago. The options available today are not the options that existed a decade ago.
If you’re ready to take the next step, the team at Apex Skin is here to help. Schedule an appointment to get an accurate diagnosis and a treatment plan built around your life.

Molly Sarkis is a licensed Physician Assistant certified by the National Commission of Certification of Physician Assistants in the state of Ohio. She grew up in Seven Hills, Ohio, and graduated summa cum laude with honors in 2018 from Cleveland State University. She received her Bachelor of Science in Health Sciences with minors in Biology and Healthcare Management.