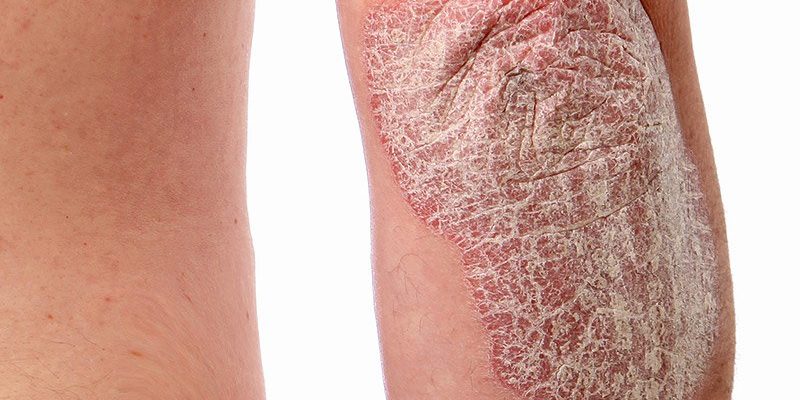
Psoriasis is a skin condition affecting over 8 million Americans and can often be hard to deal with.
Here, we’ll break down some information about psoriasis, what it looks like, how common it is, and more.
What does psoriasis look like?
Red, raised well-defined areas of skin that are covered with silvery scale.
Is psoriasis contagious?
Because this skin condition has a rash-like appearance, it can be concerning to those who aren’t familiar with it.
So, is it contagious?
“Absolutely not! Actually, patients with psoriasis are less likely to have skin infections. Unfortunately, this common misconception can be devastating for patients, especially younger children who are often ostracized from public places such as swimming pools. This misconception can be traced back to thousands of years ago when the majority of people who were put in leprosy colonies probably just had psoriasis. Whenever I see a new psoriasis patient who is worried about being contagious, I touch a psoriasis spot and then touch my face to demonstrate that I am not worried about infection.”
How is psoriasis diagnosed?
If you’re not sure if your skin condition is psoriasis, you should absolutely see a dermatologist. A misdiagnosis can lead to treatments that actually make the problem worse, not better.
In order to find out if what you have is actually psoriasis…
“Usually a dermatologist can diagnose psoriasis just by looking at your skin. Sometimes, a skin biopsy can be helpful. There are no blood tests to diagnose psoriasis.”
How common is psoriasis?
“Very common. It is estimated that psoriasis affects 2 to 3 percent of the total population, which is roughly 125 million people worldwide, including 8 million Americans who suffer from psoriasis.”
Who gets psoriasis?
Unfortunately, no specific person can be “immune” to psoriasis. In fact, it can affect everyone.
“Psoriasis can develop at any age and equally affects males and females. It is much more common in adults than children and seems to occur in two clusters: one between ages 30 and 39 and another between ages 50 and 69 years.”
What causes psoriasis?
“We still don’t know. What we do know is that a complex combination of immune, genetic, and environmental factors play pivotal roles in the disease. We know that our immune system is extremely important for properly functioning healthy skin. Normally, it takes a whole month for new skin cells to make it to the outside layer of our skin to be shed. However, in psoriasis, the immune cells make the skin cells grow too quickly and they make it to the outside layer in just one week which causes thick skin we see in psoriasis. In terms of genetics, we know that 40 percent of psoriasis patients have a first degree relative with psoriasis. We have also identified specific genes that convey an extra risk for psoriasis. Environmentally, we know smoking, obesity, alcohol, infections, and certain medications are risk factors for psoriasis or can make psoriasis worse.”
What parts of the body can psoriasis affect?
We all wish those pesky skin irritations would just stick to the areas we can cover up, right? Well…psoriasis is not one to grant that wish.
“Psoriasis can occur anywhere on the body, but some of the more common sites include the scalp, knees, elbows, belly-button and lower back. Additionally, psoriasis can affect genitals, nails, and joints. It can happen is a few small areas or involve the entire body.”
Are there different types of psoriasis?
“Yes. As dermatologists, we classically group psoriasis into six different types. In reality, there probably are even more types. Sometimes, we see patients that have a combination of multiple psoriasis types. It can be helpful to classify our psoriasis patients based on type as it can guide our treatment plans.”
These are the six most common types of psoriasis:
- Plaque psoriasis is the most common type which involves 1-10 cm sized red scaly plaques on the body.
- Guttate psoriasis usually occurs in children or younger adults without a previous history of psoriasis. Usually, these patients have a sudden eruption of many smaller red, scaly spots after strep throat.
- Pustular psoriasis can also develop quickly with multiple pustules that form over areas of red skin. This type of psoriasis can be severe and even life threatening. Pustular psoriasis can also only involve the palms and soles, which can be quite debilitating.
- Inverse psoriasis can be mistaken for a bacterial or fungal infection as it typically lacks the classic thick silvery scale. It occurs in skin folds like the armpits, inner thighs, under the breasts, and the genitals and could be quite painful
- Nail psoriasis can occur in patients with any type of psoriasis. It can range from small pits on the nails to tan-brown discolorations under the nail to even separation of the nail from the nailbed.
- Psoriatic arthritis is a type of arthritis that can cause joint pain, swelling, and morning stiffness in patients with psoriasis. It can occur in different patterns and groups of joints. Commonly, it can affect the small joints of the fingers and toes. Sometimes, the joints could swell and the finger can look like a sausage. Psoriatic arthritis can be symmetric (the right and left elbow) or asymmetric (only the right elbow). It can also involve the joints of the spine. Sometimes, without proper medical attention, psoriatic arthritis can even destroy or deform joints.
Will I get psoriatic arthritis?
One fear many have around psoriasis is conditions related to it. Will you get psoriatic arthritis if you have psoriasis?
“Maybe. About one third of people with psoriasis will have psoriatic arthritis. Most people who get psoriatic arthritis will have skin psoriasis first, often for many years before developing joint disease. Sometimes, skin psoriasis and psoriatic arthritis are diagnosed at the same time. Rarely, psoriatic arthritis is diagnosed before skin psoriasis ever appears. Dermatologists are aware of the risk of psoriatic arthritis in our psoriasis patients and question our patients about joint symptoms and examine the skin and joints at all visits. Dermatologists are also not afraid to ask for help and commonly work with joint doctors (rheumatologists) in the diagnosis and treatment of difficult psoriatic arthritis cases. We take arthritis extremely seriously as we want to prevent irreversible joint destruction.”
How severe is my psoriasis?
There are many ways to grade psoriasis severity and no way is perfect. At a minimum, we at least like to know if its mild, moderate or severe disease. Psoriasis can be graded based on the percentage of body involvement or thickness of skin plaques.
“Sometimes, it is graded based on involvement of “special sites” like scalp, face, hands, feet, and genitals. Additionally, assessing the psychosocial impact of the disease based on quality of life can be helpful. Just like we classify psoriasis by type, we also like to classify it by severity as it helps guide treatment plans.”
What other diseases are linked to psoriasis?
“Yes. We know that psoriasis is not only a disease of the skin. Recently, we learned that patients with severe psoriasis are more likely to have heart attacks and strokes, but luckily by treating the psoriasis, we can lower these risks.”
Additionally, psoriasis patients are more likely to suffer from diabetes, obesity, and liver disease. Furthermore, we know that psoriasis patients are more likely to suffer from mood disorders like depression. The profound psychosocial impact of the disease can lead to feelings of stress, low-self-esteem, and anxiety, which improve with psoriasis treatment.
Is there a cure for psoriasis?
“Unfortunately not yet. Currently, psoriasis is a lifelong condition which can improve or worsen at times. Luckily, we live in a time where we have many excellent treatments which can control psoriasis and improve quality of life.”
How can psoriasis be treated?
“This is perhaps the most exciting, yet overwhelming aspect of psoriasis as we have so many possible treatments, each with their own indications, risks, benefits, and side effects. To avoid overwhelming a new psoriasis patient it is helpful to take a simple approach.”
The treatments can be organized in four basic categories which can be used in combination or alone:
- Medicines applied to the skin, which include emollients, topical corticosteroids, and non-steroid anti-inflammatory options
- Ultraviolet light in the form of lasers, light boxes, and home-units
- Oral medications, such as methotrexate, retinoids, apremilast (Otezla), and cyclosporine
- Injectable medications, which are commonly referred to as “biologics” such as etanercept (Enbrel), infliximab (Remicade), adalimumab (Humira), certolizumab pegol (Cimzia), ustekinumab (Stelara), secukinumab (Cosentyx), ixekizumab (Taltz), brodalumab (Siliq), guselkumab (Tremfya), tildrakizumab (Illumya), and risankizumab (Skyrizi)
With all of the treatments out there, how do you know which one to choose?
“There is no right or wrong answer as every patient’s psoriasis is different”.
Picking the best treatment plan is both an art and a science. When devising a treatment plan, it is important for the dermatologist to consider many factors, including psoriasis type, amount of body involvement, joint involvement, location of disease, patient’s other comorbidities, quality of life, psychosocial impact of disease, patient preference, and cost.
In a way, it turns into a partnership between doctor and patient in picking the best treatment for their psoriasis at that moment in time. Sometimes it can be quite frustrating for the patient and dermatologist when specific treatments do not work. Luckily, there are many other great options and with some patience and perseverance, we arrive at the right treatment plan.
Can diet or lifestyle improve psoriasis?
“Yes. As we know that smoking, drinking alcohol, and obesity tends to make psoriasis worse, we tend to recommend lifestyle modifications in addition to our psoriasis treatments.”
We typically recommend smoking cessation and limiting alcohol consumption. Additionally, we discuss the importance of weight loss through healthy diet and exercise. Although there is much research interest in possible “psoriasis diets” there is not enough evidence and data to suggest a specific diet other than trying to reduce caloric intake.
Finally, given the profound psychosocial toll that psoriasis takes on patients, we discuss ways to get help managing stress, depression, itch, relationships, work, and sleep.

Where can I learn more about psoriasis?
“My favorite patient resource is psoriasis.org. It is sponsored by the National Psoriasis Foundation and contains a wealth of patient-friendly educational information along with community forums where patients can talk to each other from all over the world and be reminded that they are not alone.”
If you’re worried about having psoriasis, make sure to book an appointment with a qualified dermatologist to help you get on a plan to treat it.